US Military The Vanguard in Refractive Surgery Research and Implementation
 More than 312,000 laser refractive procedures performed in the U.S. Air Force, Army and Navy have provided invaluable insight about laser refractive surgery to both military and civilian communities.
More than 312,000 laser refractive procedures performed in the U.S. Air Force, Army and Navy have provided invaluable insight about laser refractive surgery to both military and civilian communities.
Since the first military laser study began in 1993 and the U.S. Department of Defense adopted laser refractive surgery in 2000, military laser refractive cases have demonstrated safety, efficacy and excellent visual results when performed in appropriate patients.
Military refractive cases have also provided accurate and large sample data that can be extrapolated to the general population.
“The studies that we perform here at the Naval Medical Center San Diego are viewed by civilian ophthalmologists all over the world as a benchmark of refractive surgery research because the studies are unbiased, they’re fair, they’re balanced,” U.S. Navy Capt. David J. Tanzer, MD, said. “We’re looking at safety and efficacy of [military] war fighters, so we want to ensure that these procedures are safe. … The extrapolation of the data that we accumulate here influences how civilian surgeons perform refractive surgery all over the world.”
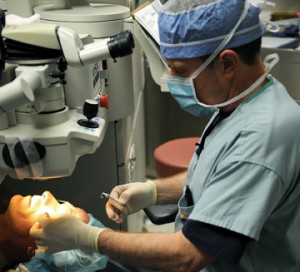
U.S. Navy Capt. David J. Tanzer, MD, performing LASIK on a patient, says that unbiased military studies of the procedure are a benchmark of refractive surgery research.
Known as a “force enhancer” or “force extender” in military parlance, refractive surgery is considered a life-saving procedure in all branches of the U.S. military. It has also helped to alter the paradigm of military medicine, according to Steven C. Schallhorn, MD.
“Refractive surgery has been revolutionary in the military,” Dr. Schallhorn said. “Nothing short of revolutionary, as far as what it can offer active duty members. Put simply, it can enhance battlefield safety and improve the performance of our military personnel.”
Refractive surgery in military
When laser refractive surgery was approved by the U.S. Food and Drug Administration, it was not permitted for enlisting military service members, but a system of waivers now allows for the procedure. The Air Force was the first military branch to waive both PRK and LASIK for all personnel, including LASIK for aviators.
The Navy and Marines Corps waive PRK and LASIK for military personnel, but not for aviators. However, those on active naval flight duty can have successful PRK procedures waived, and LASIK can be performed if service members enroll in the ongoing LASIK aviator study at the Naval Medical Center San Diego.
In the Army, both PRK and LASIK are waived for most service personnel. LASIK is performed in the Army; however, surface ablation, such as PRK and LASEK, is the preferred procedure to be performed on combat-bound soldiers and others in special operations.
Laser refractive surgery for active military personnel is now supported by the Department of Defense and top military commanders. There are six active laser refractive centers in the Air Force, 10 such centers in the Army and seven in the Navy.
Military laser refractive surgery is voluntary and based on FDA guidelines for patient selection. Patients are carefully screened and provided a detailed informed consent before refractive surgery, the same as with civilian populations.
All branches of the military adhere to specific standardized clinical guidelines for screening, examining and performing refractive surgery and following patients postoperatively. Outcomes of numerous clinical trials conducted in the military have served to hone this process to improve the outcomes of treatment performed on military members.
The most common laser procedure performed in all branches of the military is PRK, while LASIK has been gaining in popularity in recent years. In some Army laser refractive centers, up to 30% of procedures are LASIK, and at the Naval Medical Center San Diego, more LASIK procedures are performed than PRK, at a rate of 2-to-1, according to Dr. Tanzer.
Key study results
Quality of vision after refractive surgery was one of the most important factors first examined by military studies, Dr. Schallhorn said. Military research has studied thousands of patients and found excellent results even among large subject sets.
At the Naval Medical Center San Diego alone, more than 45 studies have been conducted, 15 of those with investigational device exemption from the FDA. An ongoing study there is examining 300 aviators on active flight duty — including 100 pilots — who are undergoing wavefront-guided LASIK with a femtosecond laser. So far, 175 aviators have undergone refractive surgery, Dr. Tanzer said, and approximately 50 of those are in control of an aircraft.
The study is examining the safety and efficacy of the procedure for potential approval in naval aviators, he said.
Results have shown that at 2 weeks, all aviators have 20/20 or better uncorrected vision. Of those, 96% are 20/16 and 75% are 20/12.
“The data that we have received thus far from this study is unbelievably good. It’s the best that I’ve ever seen reported or presented anywhere in the world,” Dr. Tanzer said. “Our nearsighted aviators are eligible to return to flight status by 2 weeks following refractive surgery now.”
Military studies have investigated topics such as patient-reported outcomes after surgery, contrast sensitivity, high-altitude conditions and LASIK flap exposure in high wind blasts. Studies that have investigated different laser platforms and technology without bias have also improved outcomes, Dr. Schallhorn said.
The extensive military refractive surgical experience has shown that patient selection is key to best outcomes, Dr. Reilly said. Rigorous preop screening is vital.
In addition, best postoperative results are achieved if patients use eye drops and sunglasses as directed, he said.
“The majority of the military does a lot of surface ablation, and the problems with corneal haze can really be significant if our patients aren’t educated well about how to avoid haze formation,” Dr. Reilly said.
Military results, civilian populations
Military refractive surgery demonstrates how military medicine has helped contribute to the civilian population. Dr. Reilly noted that military medicine developed the yellow fever vaccine, addressed anti-malarial and parasitic infections, and now, with refractive surgery, has changed vision enhancement.
“In the world of refractive surgery, we’ve been really trying to help advance the science and help the whole ophthalmic community understand better what’s the role of refractive surgery and what’s possible with refractive surgery,” he said. “It really is a very synergistic relationship between the military and the civilian community when it comes to refractive surgery.”
Dr. Barnes said that even though PRK is considered a more painful procedure than LASIK, Army personnel have rated pain from the procedure on a scale of 0 to 10 as a “2” at 1 day after surgery. Service members do not have a higher threshold for pain than civilians, Dr. Barnes said, and will tell physicians when they are unhappy with surgical results.
“Soldiers are like a slice of the civilian community as that is where they come from; there are tough people who wouldn’t complain at anything and there are others who seem not to tolerate almost any irritant,” he said.
In addition, almost uniformly, most military patients consider their postoperative refractive results outstanding. While there are those who occasionally complain, he said, “we have not had to discharge anybody from the Army due to a poor result or complication of refractive surgery.”
The nonmilitary community has sought out military commentary on refractive surgery. In 2008, Dr. Tanzer and Dr. Barnes spoke at an FDA Ophthalmic Device Panel meeting that examined the use of LASIK. The panel reviewed topics such as procedure safety and patient satisfaction after there were syndicated reports of patient depression and suicide after LASIK.
Dr. Tanzer presented Navy results and the military perspective on laser refractive surgery, while Dr. Barnes, who had PRK in the military before he became an ophthalmologist, spoke about LASIK and excellent patient satisfaction results. He also presented studies in military populations that have shown refractive surgery is a safe and effective procedure.
“We [military ophthalmologists] make no money if we do no laser cases at all, if we do a thousand laser cases; we make the exact same amount of money. It is of zero dollar interest to us. In fact, our life would be easier for us if we didn’t do it. We’d have less work to do. But our population is so clearly in favor of this, so happy with this and wants this, and says it’s a need for them,” Dr. Barnes said. “It’s pretty strong, being able to say things from that perspective.”
Although the Army mainly performs PRK, he said he appealed to the FDA to not discontinue the use of LASIK for military personnel because of the growing number of LASIK done in their centers.
“These soldiers, these sailors, these marines, these airmen, they are doing jobs that are now more secure,” he said. “This changes their lives. In some cases, it’s a difference between life and death.”– by Erin L. Boyle
References:
- Hammond MD, Madigan WP Jr, Bower KS. Refractive surgery in the United States Army, 2000-2003. Ophthalmology. 2005;112(2):184-190.
- Rabin J. Refractive surgery in the military. Tri-Service Vision Conservation and Readiness Program Web site. http://chppm-www.apgea.army.mil/doem/vision/army/RF_surgery/refsurginmil.ppt. Accessed Feb. 24, 2009.
- Schallhorn SC, Blanton CL, Kaupp SE, et al. Preliminary results of photorefractive keratectomy in active-duty United States Navy personnel. Ophthalmology. 1996;103(1):5-22.
- Col. Scott D. Barnes, MD, is stationed at Womack Army Medical Center, Fort Bragg, NC 28310. He can be reached at COL Scott Barnes, Dept. of Ophthalmology-WAMC, Fort Bragg, NC 28310; 910-907-7921; e-mail: scott.d.barnes@us.army.mil.
- Lt. Col. Charles D. Reilly, MD, can be reached at 59 SSS/SGO2E, Wilford Hall USAF Medical Center, Lackland AFB, 2200 Bergquest Drive, Suite 1, San Antonio, TX 78236-5300; 210-292-2010; fax: 210-292-2313; e-mail: charles.reilly@lackland.af.mil.
- Steven C. Schallhorn, MD, can be reached at scschallhorn@yahoo.com.
- Capt. David J. Tanzer, MD, can be reached at Naval Medical Center San Diego, 34800 Bob Wilson Drive, San Diego, CA 92135; 619-532-6700; e-mail: david.tanzer@med.navy.mil.
Share This